Choosing the right MSPs means that they understand the proper functioning of an organization and know how to deal with issues, especially in the healthcare sector, and how high the stakes are during every procedure.

Many healthcare administrators and organizations don’t think seriously about their IT provider until it’s too late and something breaks.
A server going down at midnight, an EHR system failing mid-shift, or a ransomware locking staff out of patient records can have disastrous effects on the healthcare operations, with the stakes always being so high.
This guide explains how your organization can avoid these mistakes and choose a reliable managed IT service provider (MSP) to assist in your workflow operations and decisions.
Key Takeaways
- Verifying the claims of an MSP by asking smart questions about their experiences
- Ensuring that your MSP prioritizes cybersecurity actions and is willing to take the necessary steps to enforce it
- Making sure that an IT service provider can assist with the scalability of your organization by providing the needed requirements
- The things that separate a real healthcare MSP from a generalist pretender
Healthcare IT isn’t just regular IT with a HIPAA checkbox bolted on. It’s a distinct discipline. Your systems aren’t just storing spreadsheets – they’re keeping track of medication dosages, lab results, imaging files, and care plans.
When these systems fail, the clinical staff aren’t able to do their jobs properly. This can sometimes end up directly affecting patient outcomes.
A good MSP for healthcare needs to genuinely understand things like:
If you’re evaluating a provider and they’re not immediately comfortable talking about these things, that tells you something important.
Every managed IT service provider pitching to a client will tell you that they’re HIPAA compliant. Without the details, that phrase has become almost meaningless on its own. What you actually want to know is how they handle compliance in real operational situations.
Push them on specifics. Ask whether they’ll sign a Business Associate Agreement – they must, legally, if they’re touching anything related to protected health information. Ask when they last completed a HIPAA risk assessment and what it found. Ask what their breach notification process looks like.
The answers matter less than how they answer. A provider that’s genuinely embedded in healthcare will talk about these things fluently, with specific examples. One that’s just checking boxes will hedge and use vague language. You’ll feel the difference.
A few questions worth asking directly:

The healthcare organizations are among the most frequently attacked sectors. The reasons are straightforward: patient data is valuable, clinical systems often run outdated software, and the pressure to restore operations quickly means ransomware victims in healthcare are more likely to pay.
According to the HIPAA Journal’s 2025 ransomware analysis, healthcare remained the most targeted sector for yet another year, accounting for 22% of all disclosed attacks – and the average cost of a healthcare data breach reached $7.42 million, nearly double the global average. Attackers know this.
This doesn’t mean doom and gloom – it means your MSP needs to take security seriously as a default, not as an add-on tier. Some things to look for:
Ask these questions and tell them to describe a real incident they’ve managed for a healthcare client. Not a case study from the website – a real conversation about what happened, what they did, and what they learned. That answer will tell you a lot.
There’s a big gap between an MSP that says they support healthcare clients and one that actually knows how Epic’s upgrade cycles work, or how to troubleshoot a DICOM routing issue at 6 am before radiology opens.
The healthcare software ecosystem is sprawling and specific. EHR platforms like Epic, Cerner, or Meditech each have their own quirks, integration requirements, and support models. Imaging systems, lab information systems, pharmacy software, telehealth platforms – they all need to talk to each other, and when they don’t, you need someone who knows why.
Ask your providers which systems they’ve supported previously. If your organization runs Epic, ask for references from Epic environments.
If you’re planning a cloud migration of clinical workloads, find out if they’ve actually done that – not just a generic cloud migration, but one in a HIPAA-regulated environment.
References matter the most here than anywhere else. Healthcare is a relatively small world, and people will communicate honestly if called.
Did You Know?
While external hackers get headlines, human error, such as employees falling for phishing emails or mishandling data, remains the top cause of cyber breaches, showing a lack of IT threat aversion training.
Service Level Agreements can be written to sound impressive while promising very little. Phrases like “priority response” and “business-critical support” are meaningless without numbers attached to them.
What you need in healthcare specifically:
One thing that gets overlooked: ask how they handle scheduled maintenance on systems that can’t afford downtime.
In most industries, you can push a patch at 2 a.m., and nobody notices. In a hospital, 2 am might be the busiest time in the ED. A healthcare MSP should have a process for this.
Cloud adoption in healthcare has moved from “emerging trend” to “operational reality” over the past few years. Most organizations are somewhere on the journey – whether that’s moving email and collaboration tools to Microsoft 365, hosting EHR workloads on AWS, or building out a full hybrid infrastructure.
The main issue is that cloud migrations in the healthcare sector come with many constraints that most providers and generic MSPs underestimate.
Data residency requirements, BAAs with cloud vendors, encryption standards for PHI in transit and at rest, access controls that satisfy both clinical workflow needs and HIPAA auditors – these aren’t afterthoughts. They need to be designed in from the start.
When evaluating an MSP’s cloud capabilities, ask about specific healthcare cloud projects they’ve completed. Find out whether they have certifications on the platforms you’re considering.
Ask about their disaster recovery approach – specifically: if your primary cloud environment goes down, what’s the RTO, and have they ever tested it?
Check out this infographic to learn more about how important the use of cloud systems is for the healthcare sector:
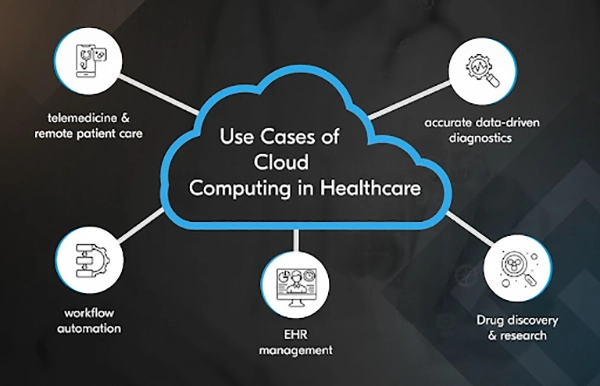
Healthcare organizations don’t stay the same size or shape. They expand, acquire facilities, and grow their networks. The MSPs you choose should be able to grow and scale with you without something breaking and falling apart every time something changes.
Ask them directly how they’ve handled growth scenarios for existing clients. If a healthcare organization they work with opened three new locations in 18 months, how did they manage the IT onboarding? What’s their process for bringing a newly acquired facility into a standardized infrastructure?
Also worth exploring: how stable is their own team? High turnover in an MSP means you’re constantly re-educating people about your environment. Ask about average tenure on their healthcare accounts. Ask whether you’d have a dedicated account manager and technical lead, or whether support comes from a rotating pool.
After going through this process with a few providers, you start to notice a pattern. The ones who really know healthcare talk about it differently. They use clinical language naturally.
They ask about your workflows, your staff pain points, and your seasonal patient volume. They know what a CAH is. They’ve heard of HL7 before you mentioned it.
The generalists, on the other hand, talk mostly about uptime, ticket resolution times, and their security stack. Those things matter – but they’re not the full picture.
Providers that specialize in the healthcare sector, like Svitla Systems healthcare MSP, bring something generalists can’t replicate: a working knowledge of how healthcare organizations actually function, built from real client experience in the sector.
That knowledge shows up in different ways that matter a lot. It’s the difference between a person who understands why you can’t just restart a workstation mid-shift and one who does it anyway because an update needs to go out.
A few things that should give you pause during evaluation:
None of these is automatically disqualifying on its own. But a pattern of them is.
Healthcare IT decisions tend to get made under pressure – after an incident, during a budget cycle, or when a contract is expiring. That’s exactly the wrong time to do a thorough evaluation.
The organizations that end up with the best MSPs are usually the ones that planned the process beforehand and gave themselves enough time, treating the selection like a strategic decision, which it actually is.
Do the reference calls. Sit in on a technical demo. Ask the uncomfortable questions about past failures and how they were handled. The sales team will always put their best foot forward – what you’re really trying to find out is who shows up at 3 am when something goes wrong.
In healthcare, that question has a real answer, and it matters.
Choosing the right MSPs means that they understand the proper functioning of an organization and know how to deal with issues, especially in the healthcare sector, and how high the stakes are during every procedure.
A verified experience in the same sector shows that they know what they’re doing and understand the implications that come with its operations.
Yes, healthcare organizations are the most targeted sector out of any, and a stoppage in their processes directly influences a patient’s procedure, making cybersecurity essential.
Yes, an MSP is directly responsible for influencing the scalability of an organization, as they provide the assets and systems to help achieve the desired outcomes.
